South Africa’s Eastern Cape Department of Health collaborated with Spark Health Africa in 2012 to embark on a Transformative Leadership and Culture Change (TLCC) initiative. Using the competencies that they developed as part of this initiative the provincial management team improved stock availability of all medicines and supplies from 54% to 95% over a six-month period.
This article outlines the approach that the team adopted to understand the underlying causes of stock-outs and to enhance support and supervision of personnel at the depots to achieve this improvement in-stock availability.

Why is the supply of essential medicines important?
Essential medicines are critical to satisfying the priority health care needs of a population. As the shift towards Universal Health Coverage gains momentum, the role of essential medicines is integral to delivering health services to all without imposing financial hardships on individuals.
Eastern Cape, the third most populous province in South Africa, used to be plagued by chronic shortages of essential medicines and supplies. Shortages were driven by ineffective leadership and lack of accountability across the health system.
During this time, the Provincial Department of Health was acutely affected by reports of medicine and medical supply shortages. Depot managers sent bi-weekly reports on stock levels to the national and provincial offices indicating that medicine levels had been consistently low since September 2012. Levels were especially low for drugs to treat HIV, TB, vaccines and tracer medicines. (Tracer medicines are select medicines which are tracked as part of routine monitoring to measure healthcare delivery performance in regard to supply and availability of drugs)
While a number of reasons were stated for low stock availability, the main causes were delays and irregular deliveries from suppliers, and ordering delays by the pharmaceutical storage depots. A report dated February 2013 from the pharmaceutical depots showed that the province had 54% availability of tracer medicines against a target of 100% availability.
Low stock availability at the depots negatively impacted the supply at facility level which resulted in treatment interruptions. Such interruptions were most acute for patients with chronic diseases like HIV & AIDS, TB, hypertension, and diabetes. Health facilities were also unable to enroll new patients and retain them on chronic programs due to the low medicine stock availability. Consequently, the province could not meet national targets to increase enrollment and retention of HIV positive patients on antiretroviral therapy.
Leadership in the Provincial Department of Health viewed addressing the root causes of the acute shortage of medicines as critical to improve service delivery. The provincial team decided to focus on improving the availability of medicines and consumables at the two main depots of Mthatha and Port Elizabeth as part of their transformative journey with Spark Health Africa.
How did the team address essential medicines stock outs?

Setting up a Multi-disciplinary team
The provincial team was composed of managers from multiple disciplines. Given the complex nature of the health system, a multi-disciplinary approach ensured the problem was addressed comprehensively. Each manager, whether clinical or non-clinical, had a role to play. They were unified by the negative impact stock-outs had on each of their key performance areas.
Igniting a mindset shit to view work differently
Spark Health Africa supported teams to think differently about their work during a five-day igniting workshop and 12 months of subsequent mentoring and thought partnership. Instead of focusing on the problems and potential barriers to addressing stock-outs, the team shifted attention to understand the nature and extent of the problem using data and to devise solutions.
Leadership commitment and support was key to addressing stock outs. Using a process of discovery, the Spark Health Africa mentors guided the team to identify pressure points that could lead to support from the leadership. The challenge of stock outs had become a highly sensitive and political issue making news headlines on several occasions and casting the leadership in bad light. To push forward their agenda, the team leveraged the negative publicity as well as the need to demonstrate competency by one of the heads of department who was in an acting role. To this end, the team engaged the provincial executive management team, which included technical and political leadership. The support gained from top leadership opened the doors to the two depots for the team to undertake an analysis of the underlying causes of stock outs.
Using the Spark Health Africa approach to structured problem solving, the team developed an evaluation tool to facilitate analysis of the value chain and to understand the root causes to stock outs. This tool assessed several factors that affect medicine availability. These included the depot infrastructure, staff complement, budget availability, supplier management and customer management.
Low stock availability root causes and interventions
The assessment revealed poor inventory management and lack of supervision (and therefore accountability) of stocks by depots. Submission of reports showing the status of stock availability in the depots was done on an ad-hoc basis, yet this was supposed to be a routine process. Also, there was poor recording, inefficient logistics processes and poor management of contracts with suppliers. The assessment also exposed that the supply chain disruptions had resulted in some medicines expiring while still held in the depots.
The assessment also brought to light a severe shortage of human resources, worsened by a directive preventing new recruitments. Mthatha depot in particular had been severely affected by the shortage in human resources to the extent that many administrative functions had been taken over by Port Elizabeth depot. This included processing of orders with suppliers and the financial management processes. As a result, Mthatha had become more of a logistical warehouse than a fully functional depot. However, analysis of the work-flow indicated that the two depots worked similarly and therefore there was no plausible justification for Mthatha depot to be less adequately resourced than Port Elizabeth depot.
The Mthatha depot, therefore, became the main focus of the intervention. One of the eight districts in the province, the OR Tambo district, was identified for piloting interventions at both district and facility levels given the magnitude of the perennial stock outs reported by this district.
What interventions were implemented?
Several interventions were implemented and these included:
- Immediate placement of community service pharmacists in Mthatha depot with plans to increase this cadre every year
- Creation of additional capacity through re-assignment of community health workers at Mthatha depot to assist with picking and packing stock at the depots.
- Re-purposing of auxiliary workers as pharmacist assistants in facilities across OR Tambo district. These pharmacist assistants were given orientation and training to take on the responsibility to manage medicines in clinics.
- Streamlining of ordering processes to allow for ordering by facilities directly to the depot.
In an unprecedented move to drive accountability, health facilities were also asked to produce weekly reports on stock availability, the number of patients on ART and orders placed with the depots. The weekly reports produced by facilities allowed for timeous identification of facilities facing stock-outs. These reports were shared with senior management and discussed in senior management meetings.
Intervention outcomes
Six months into implementation, the medicine availability at the depot had increased to 95% from a baseline of 54%.
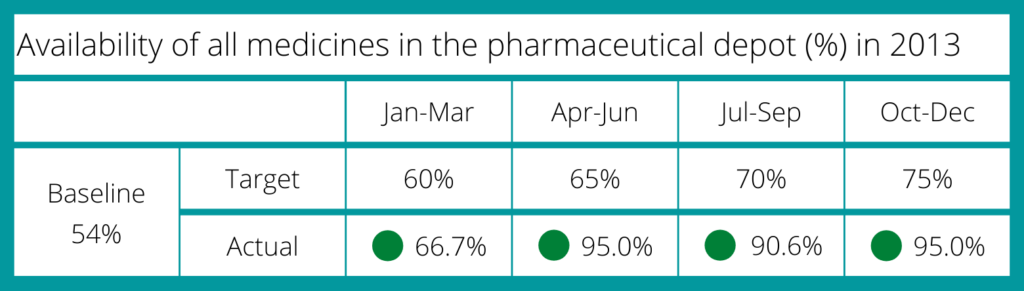
The team achieved their initial target ahead of schedule, and as such, they were able to shift focus towards providing support at facility level, thus ensuring that facilities are able to maintain adequate stock levels of essential medicines i.e. chronic medicines, ARVs Anti TB medicines and vaccines.
Lessons learned
- Teamwork must be encouraged across functions and disciplines to unlock system wide interventions
- Identifying and engaging the right stakeholders creates an enabling environment for implementation
- Timely data, reviewed by the appropriate stakeholders is effective in driving accountability
- Applying a systematic and structured approach assists in problem solving even when faced by seemingly complex issues
- Inventory management requires both technical and behavioral components to be addressed simultaneously
